|
In a study by Gerigk 9 of 103 children admitted to the hospital with acute medical illnesses, the median plasma Na value was 136 mmol/L, with plasma ADH levels that were higher than would be expected for that degree of hyponatremia. It is therefore not surprising that mild degrees of hyponatremia are a common finding in pediatric patients receiving parenteral fluid therapy. However, nonphysiologic stimuli for antidiuretic hormone (ADH) secretion, which inhibits excretion of EFW (e.g., pain, anxiety, narcotics, positive-pressure ventilation), are common in critically ill patients. Although convenient and simple to use, the assumptions made about daily requirements for sodium, potassium, and EFW mandate the use of hypotonic intravenous (IV) solutions, which has been almost universal practice in pediatric medicine for almost 50 years ( Table 113-4). This paper by Holliday became the standard reference text for parenteral fluid administration in pediatrics. TABLE 113-3 Requirements for Maintenance Parenteral Fluids* The estimates for Na (3 mmol/100 kcal/d) and K (2 mmol/100 kcal/day) in maintenance fluids were calculated from the sodium and potassium concentration of cow’s milk and breast milk. Factoring in water of oxidation of 16.7 mL/100 kcal/d leaves a total of 100 mL/100 kcal/d for replacement of normal losses. 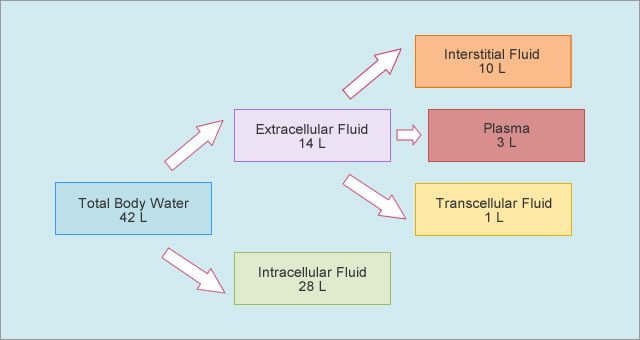
An allowance of 100 mL/100 kcal/d was made for insensible water loss, with 66.7 mL/100 kcal/d to replace urine output. 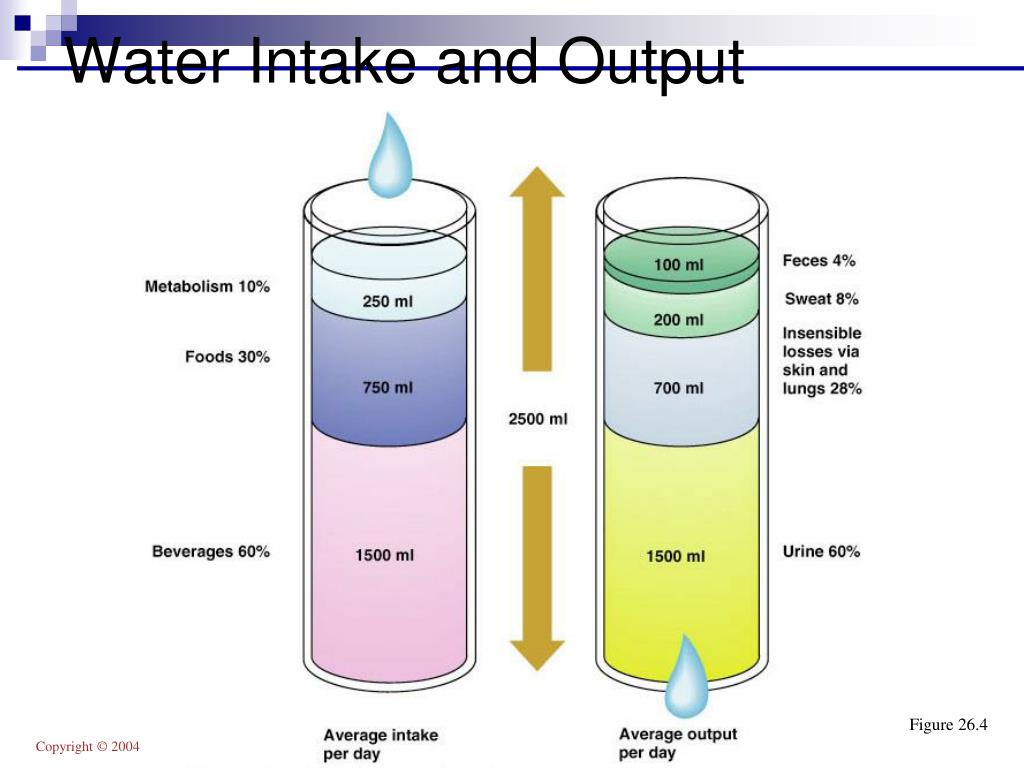
In 1957, Holliday 8 published a formula that linked body weight to energy expenditure ( Table 113-3). When oral intake is replaced by parenteral fluids in children, the amount of fluid (i.e., water) given depends on body weight and energy expenditure. Infants and small children are unable to regulate their intake because they do not have access to water for the same reasons that apply in older children or adults in coma or with reduced levels of consciousness. In the normal healthy individual, water intake is regulated by thirst stimulated via osmoreceptors in the hypothalamus. However, in critically ill children, urinary Na and K concentration may be much higher. This assumes that these are the amounts of cations needed for normal homeostasis. The commonly used values for sodium (Na) and potassium (K) requirements in parenteral fluids in children are 2 to 3 mmol/kg/d and 1 to 2 mmol/kg/d. Urine is the major source of electrolyte loss in the body except when there are fluid losses from the gastrointestinal tract. Typically this occurs in gastroenteritis, where reduced oral intake is combined with excessive water and electrolyte loss in the stool. High solute load and limited urine concentrating ability makes them prone to significant ECF contraction (dehydration) when there are excessive amounts of water loss. In addition, the infant’s high metabolic rate and the solute load from enteral feeding formula means they require more water excretion per unit solute amount. 2 Infants are somewhat disadvantaged compared to the older child and adult in that they cannot maximally dilute (infant 200 mOsm/L versus adult 80 mOsm/L) and concentrate urine (infant 800 mOsm/L versus adult 1200 mOsm/L). The average osmolar excretion in newborn infants receiving infant formula is 16 to 20 mOsm/kg/d. Obligate water excretion in the urine is dependent upon solute load and the ability to concentrate and dilute urine. 
TABLE 113-2 Water Losses in Normal Children (mL/100 kcal/24 h) 4 – 7 Further discussion of fluid and electrolyte physiology in the preterm infant is beyond the scope of this chapter. 3 In addition, glomerular filtration rate is lower than in the term infant, and the large surface area–to–body weight ratio leads to considerable evaporative losses. 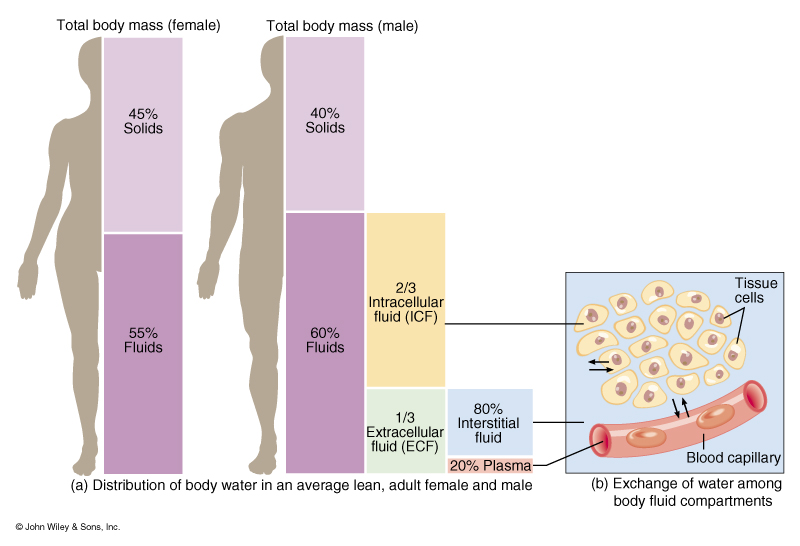
Fractional excretion of sodium is inversely correlated with age in the preterm, who is susceptible to both sodium loss and sodium and volume overload. The preterm infant has a relative expansion of both TBW and ECF volume expansion, and a diuresis in the first few days of postnatal life is a common finding. By term, ECF and intracellular fluid (ICF) volume has fallen to 45% and 30% of TBW, respectively ( Figure 113-1). During early fetal life, TBW represents 90% of total body weight, with 65% being in the extracellular fluid (ECF) compartment. 1, 2 Total body water (TBW) is high in the fetus and preterm infant. Body water content changes significantly with age in children.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
